SLEEP APNEA
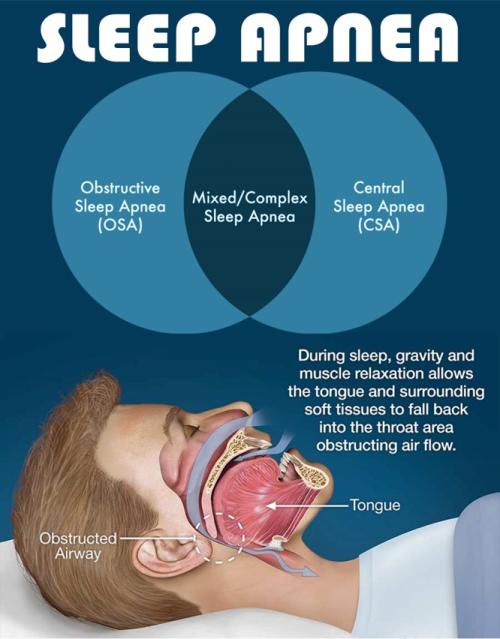
Sleep apnea is a sleep disorder characterized by pauses in breathing or shallow breathing during sleep. These pauses can last for a few seconds to minutes and can occur multiple times per hour. There are two main types of sleep apnea: obstructive sleep apnea (OSA) and central sleep apnea (CSA). Additionally, some individuals may have a combination of both, known as complex or mixed sleep apnea
Obstructive Sleep Apnea (OSA): OSA is the most common type of sleep apnea and occurs when the muscles in the throat relax excessively during sleep, leading to partial or complete blockage of the upper airway. This obstruction results in pauses in breathing and disrupted airflow. OSA is often characterized by loud snoring, gasping or choking sensations during sleep, and daytime sleepiness or fatigue. Risk factors for OSA include obesity, older age, male gender, family history, smoking, alcohol use, and anatomical factors such as enlarged tonsils or a narrow airway.
Central Sleep Apnea (CSA): CSA occurs when the brain fails to send the appropriate signals to the muscles responsible for controlling breathing during sleep. Unlike OSA, there is no physical obstruction in the airway with CSA. Instead, breathing pauses occur due to instability in the respiratory control center of the brain. CSA is less common than OSA and may be associated with certain medical conditions such as heart failure, stroke, brainstem lesions, or opioid use.
Complex or Mixed Sleep Apnea: Complex sleep apnea, also known as mixed sleep apnea, involves a combination of obstructive and central sleep apnea. Individuals with complex sleep apnea may experience features of both types of apnea, with periods of obstructive events followed by central events or vice versa.
Symptoms
The symptoms of sleep apnea can vary depending on the type and severity of the condition. Common signs and symptoms may include:
Loud or Disruptive Snoring: Particularly with OSA, loud and persistent snoring is a common symptom.
Pauses in Breathing During Sleep: Witnessed by a bed partner or family member, these pauses may be followed by gasping, choking, or snorting sounds.
Excessive Daytime Sleepiness: Feeling tired or fatigued during the day, even after a full night's sleep.
Morning Headaches: Waking up with a headache or feeling groggy upon awakening.
Difficulty Concentrating or Memory Problems: Impaired cognitive function or difficulty concentrating due to poor sleep quality.
Irritability or Mood Changes: Feeling irritable, moody, or experiencing mood swings due to sleep disturbances.
Dry Mouth or Sore Throat: Waking up with a dry mouth or sore throat may indicate mouth breathing during sleep, which can be associated with sleep apnea.
Frequent Nighttime Urination: Nocturia, or the need to urinate frequently during the night, may be a symptom of sleep apnea, particularly in individuals with OSA
Diagnosis & Treatment
It's important to note that not everyone with sleep apnea will experience all of these symptoms, and some individuals may not be aware of their breathing disturbances during sleep. Untreated sleep apnea can lead to serious health complications, including hypertension, heart disease, stroke, diabetes, and cognitive impairment. Therefore, it's essential to seek evaluation and treatment if you suspect you or someone you know may have sleep apnea. A healthcare provider can conduct a comprehensive evaluation, which may include a sleep study (polysomnography), to diagnose sleep apnea and recommend appropriate treatment options. Treatment for sleep apnea may include lifestyle modifications, such as weight loss or positional therapy, continuous positive airway pressure (CPAP) therapy
BREATHING TROUBLE
Breathing difficulties, also known as dyspnea, can be caused by various factors and may range from mild to severe
Respiratory Conditions
Asthma: A chronic respiratory condition characterized by inflammation and narrowing of the airways, leading to wheezing, shortness of breath, and chest tightness.
Chronic Obstructive Pulmonary Disease (COPD): A group of progressive lung diseases, including emphysema and chronic bronchitis, that cause airflow obstruction and breathing difficulties.
Pneumonia: Infection and inflammation of the lungs, often caused by bacteria, viruses, or fungi, leading to symptoms such as cough, fever, chest pain, and difficulty breathing.
Pulmonary Embolism: Blockage of the pulmonary artery or its branches by a blood clot, causing sudden onset of shortness of breath, chest pain, and rapid heart rate.
Pulmonary Edema: Accumulation of fluid in the lungs, often due to heart failure, leading to symptoms such as difficulty breathing, coughing, wheezing, and frothy sputum.
Interstitial Lung Disease: A group of disorders characterized by inflammation and scarring of the lung tissue, leading to progressive dyspnea and decreased lung function.
Cardiovascular Conditions
Heart Failure: Inability of the heart to pump blood effectively, leading to fluid buildup in the lungs (pulmonary congestion) and symptoms such as shortness of breath, fatigue, and swelling of the legs.
Heart Attack: Blockage of blood flow to the heart muscle, leading to chest pain, shortness of breath, nausea, and sweating.
Arrhythmias: Irregular heart rhythms, such as atrial fibrillation, can cause inadequate blood flow to the body and lead to symptoms such as palpitations, chest discomfort, and shortness of breath.
Other Medical Conditions
Anemia: Decreased red blood cell count or hemoglobin levels, leading to reduced oxygen-carrying capacity of the blood and symptoms such as fatigue, weakness, and shortness of breath.
Obesity: Excess body weight can put pressure on the chest and abdomen, making it difficult to breathe, especially during physical activity.
Anxiety or Panic Attacks: Psychological factors such as stress, anxiety, or panic attacks can cause hyperventilation or rapid breathing, leading to feelings of breathlessness, chest tightness, and dizziness.
Symptoms
PULMONARY DISEASES
Chronic Obstructive Pulmonary Disease (COPD) Smoking is the primary cause of COPD, with long-term exposure to cigarette smoke leading to inflammation and damage to the airways and lung tissue. Other risk factors include exposure to air pollution, occupational dusts and chemicals, genetic factors (alpha-1 antitrypsin deficiency), and respiratory infections.
Asthma Asthma is a chronic inflammatory condition of the airways, with a complex interplay of genetic and environmental factors contributing to its development. Triggers such as allergens (pollen, dust mites, pet dander), respiratory infections, air pollution, exercise, cold air, and certain medications can cause airway inflammation and bronchoconstriction in susceptible individuals.
Pneumonia Pneumonia is often caused by bacterial, viral, fungal, or parasitic infections. Streptococcus pneumoniae is the most common bacterial cause of pneumonia, while viruses such as influenza and respiratory syncytial virus (RSV) are common viral causes. Other factors that can increase the risk of pneumonia include smoking, chronic lung diseases, weakened immune system, age (young children and older adults), and certain medical conditions such as heart disease or diabetes.
Tuberculosis (TB) Tuberculosis is caused by infection with Mycobacterium tuberculosis bacteria. It primarily affects the lungs but can also affect other parts of the body. TB is spread through the air when an infected person coughs, sneezes, or speaks. Factors such as close contact with an infected person, weakened immune system (HIV/AIDS, malnutrition), and living or working in crowded or unsanitary conditions increase the risk of TB transmission.
Lung Cancer Lung cancer is primarily caused by long-term exposure to carcinogens such as tobacco smoke, including firsthand and secondhand smoke. Other risk factors include exposure to radon gas, asbestos, arsenic, certain metals, and air pollution. Genetic factors, family history, and pre-existing lung diseases may also increase the risk of lung cancer.
Interstitial Lung Disease (ILD) Interstitial lung diseases are a group of disorders characterized by inflammation and scarring (fibrosis) of the lung tissue. Causes of ILD include environmental exposures (such as occupational dusts, chemicals, or asbestos), certain medications (e.g., chemotherapy drugs, immunosuppressants), autoimmune disorders (e.g., rheumatoid arthritis, systemic sclerosis), infections, and genetic factors.
Pulmonary Embolism (PE) Pulmonary embolism occurs when a blood clot (usually from the deep veins of the legs) travels to the lungs and blocks blood flow in the pulmonary arteries. Risk factors for pulmonary embolism include prolonged immobility, surgery, trauma, obesity, pregnancy, cancer, hormonal therapy, genetic predisposition (thrombophilia), and certain medical conditions such as heart disease or chronic lung diseases.
Chronic Bronchitis Chronic bronchitis is a type of COPD characterized by inflammation and irritation of the bronchial tubes. Smoking is the primary cause of chronic bronchitis, with long-term exposure to tobacco smoke leading to chronic inflammation and mucus production in the airways. Other factors such as air pollution, occupational exposures, and respiratory infections can also contribute to chronic bronchitis.
Pulmonary Fibrosis Pulmonary fibrosis is a progressive lung disease characterized by scarring (fibrosis) of the lung tissue, which makes it difficult for the lungs to function properly. The cause of pulmonary fibrosis is often unknown (idiopathic), but it can be associated with environmental exposures (such as asbestos, silica, or certain medications), autoimmune disorders, genetic factors, infections, or occupational exposures
